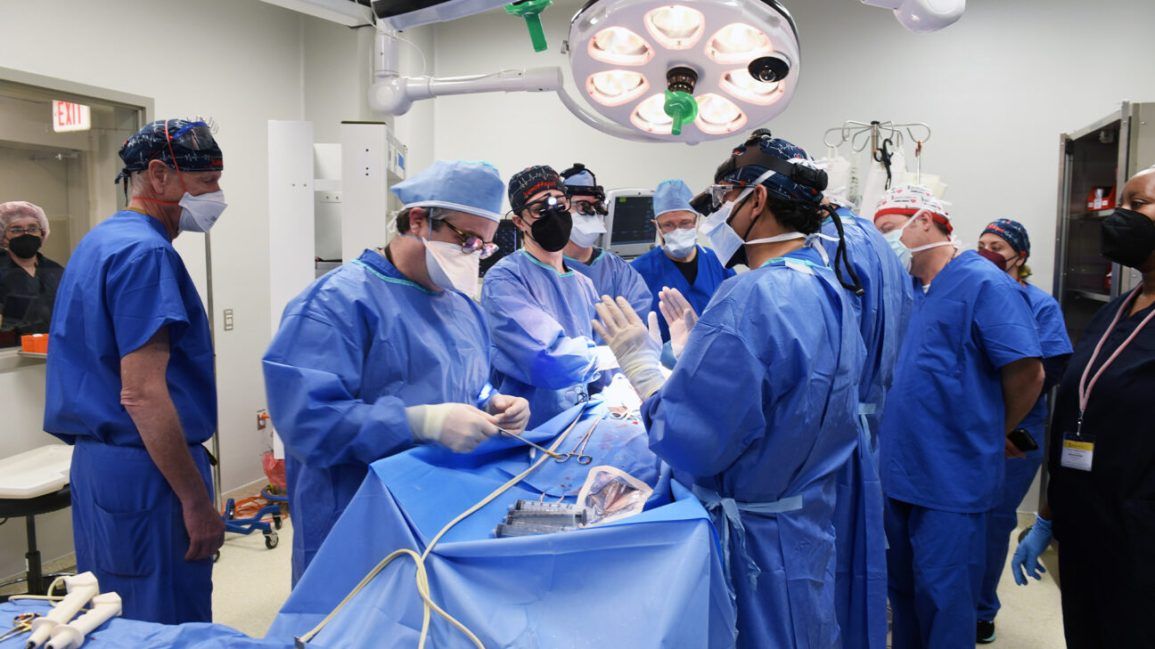
A medical team at the University of Maryland Medical Centre in the United States carried out the operation in just over 8 hours. Scientific director of the xenotransplantation unit at the university Dr Muhammad Mohiuddin said that “if this works, there will be an endless supply of these organs for patients who are suffering”.
David Bennet was the terminally ill 57-year-old man who received the GMO pigs’ heart and said that “it was either die or do this transplant” while adding further “I know it’s a shot in the dark, but it’s my last choice” he said before the surgery. Xenotransplantation has been around for many years with previous failed attempts including the transplantation of a baboon heart into a baby in 1984 which resulted in the infant dying 21 days later.
The so far success of this xenotransplantation is giving doctors hope that patients waiting on organ transplant lists will significantly reduce. As of April 2021, there are currently 1600 people waiting for an organ transplant in Australia with approximately only 1300 deaths a year eligible to donate their organs, as they must die in hospital on ventilation.
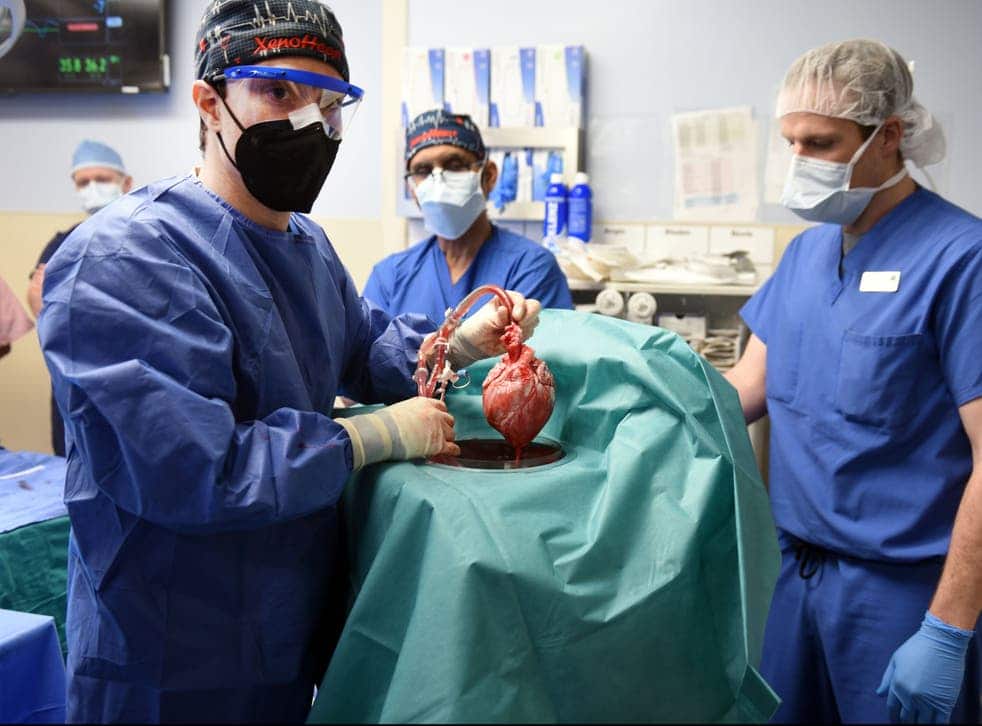
“The first heart xenotransplantation was chimpanzee to human in 1964 – rejection was so severe that it was only tried a couple more times before being abandoned,” he said.
“Even with a good matching human-human transplant, we need multiple drugs to immunosuppress and prevent rejection – this obviously exposes the recipient to serious infections, including Covid-19,”
“For many years, we have used pig heart valves in humans, but these valves have first been rendered non-antigenic i.e., there is no protein material left in them to create a rejecting antibody response,”
“Genetic modification of pig donor hearts therefore makes a lot of sense, so that the genes, or DNA do not make foreign proteins that will be rejected,”
“Given the world-wide shortage of human donor hearts, and especially in Australia, this has the potential for being a major breakthrough, allowing many more people to get this potentially fantastic treatment for severely failing hearts.”
While internationally recognised heart transplant researcher and University of New South Wales Professor Peter Macdonald also told NewsCop that this will no doubt be helpful in other areas of organ transplants.
“This [xenotransplantation] also applies to transplantation of other organs and tissues e.g., kidney, liver, lung, pancreas including pancreatic islets,” he said.
“So, the clinical implications of this transplant if successful are potentially huge.”
Doctors will be closely monitoring Mr Bennet in the coming days and weeks to ensure the continued success of the xenotransplantation.